Report Materials
Why OIG Did This Audit
- Applied Behavior Analysis (ABA) is a therapeutic approach for managing the symptoms of autism and other developmental disabilities, usually centered on improving social and communication skills.
- In the past several years, Federal and State agencies have identified questionable billing patterns by some ABA providers and payments to providers for unallowable ABA services.
- Colorado’s fee-for-service (FFS) Medicaid payments for ABA in 2019 were $60.1 million, and by 2023 these payments had increased to $163.5 million.
- This audit examined whether Colorado’s FFS Medicaid payments for ABA for 2022 and 2023 complied with Federal and State requirements.
What OIG Found
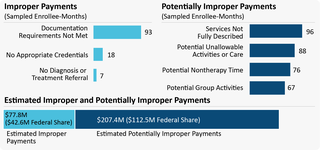
Colorado’s payments for ABA did not fully comply with Federal and State requirements. All 100 sampled enrollee-months included payments for 1 or more claim lines that were improper or potentially improper.
What OIG Recommends
We made five recommendations, including that Colorado refund $42.6 million to the Federal Government, provide additional guidance to ABA facilities for documenting and billing ABA, and periodically perform a statewide postpayment review of Medicaid ABA payments to educate providers on requirements. The full recommendations are in the report.
Colorado disagreed with one recommendation. Colorado agreed with three recommendations, partially agreed with one recommendation, and detailed steps it has taken and plans to take in response to our recommendations.
View in Recommendation Tracker
Notice
This report may be subject to section 5274 of the National Defense Authorization Act Fiscal Year 2023, 117 Pub. L. 263.