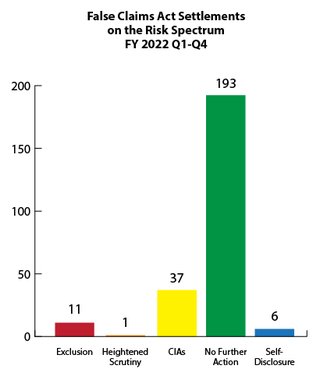
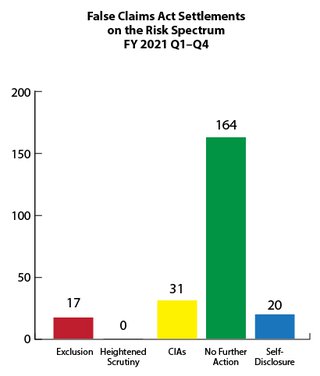
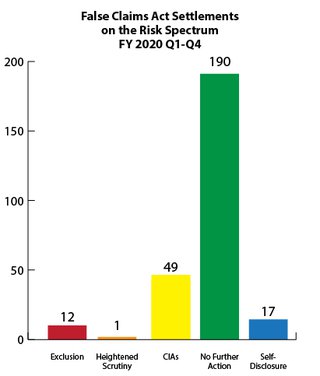
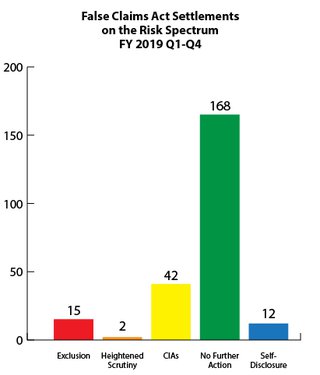
Fraud Risk and Heightened Scrutiny
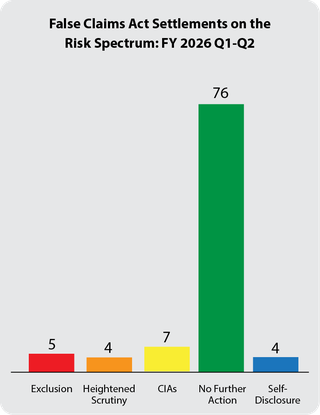
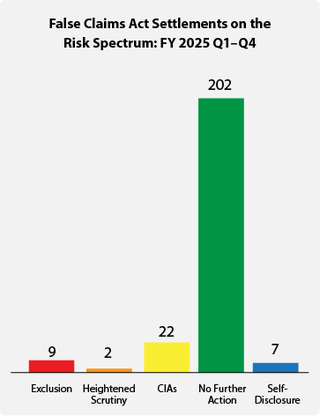
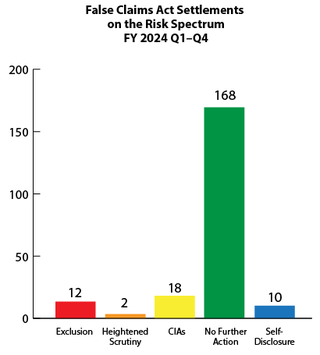
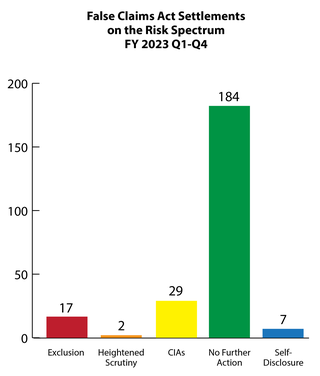
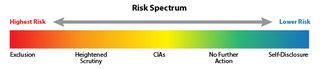
The government's primary civil tool for addressing health care fraud is the False Claims Act (FCA). Most FCA cases are resolved through settlement agreements in which the government alleges fraudulent conduct and typically the settling parties do not admit liability. Depending on the facts and circumstances presented, OIG will usually pursue one of the following approaches when settling a health care fraud case: (1) exclusion; (2) heightened scrutiny; (3) integrity obligations; (4) take no further action; or (5) in the case of a good faith and cooperative self-disclosure, release 1128(b)(7) exclusion with no integrity obligations. OIG’s Risk Spectrum illustrates these approaches. For more information on how OIG evaluates risk to the Federal health care programs and the criteria the OIG considers in evaluating exclusions in False Claims Act cases, see OIG’s April 18, 2016 notice.
Risk Spectrum Category Links
- Exclusions Program
- Parties Under Heightened Scrutiny
- Corporate Integrity Agreements
- Self-Disclosure Information
FY 2026 Q1-Q2
Last updated April 28, 2026